Insurance commissioner warns network disputes could rise, outlines bills to protect patients
January 23, 2026 | Finance Committee, SENATE, SENATE, Committees, Legislative, Maryland
This article was created by AI summarizing key points discussed. AI makes mistakes, so for full details and context, please refer to the video of the full meeting. Please report any errors so we can fix them. Report an error »
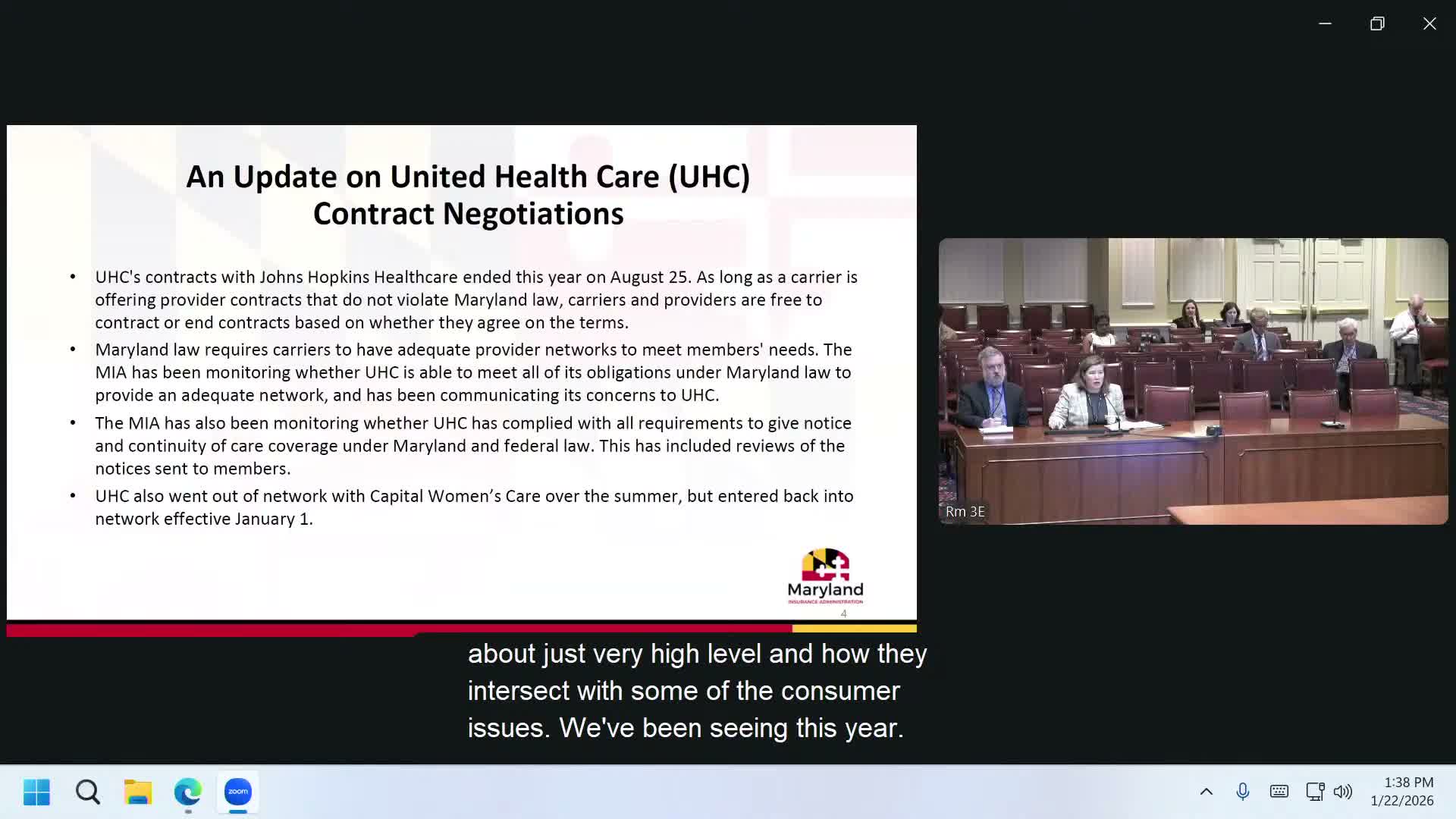
Maryland Insurance Commissioner Marie Grant told the Senate Finance Committee on Jan. 22 that contract disputes between large health systems and carriers — notably UnitedHealthCare and Johns Hopkins — left many patients at risk and prompted departmental proposals to strengthen consumer protections.
"As a regulatory agency, we can't force parties to contract," Grant said, recounting that the United–Johns Hopkins contract ended Aug. 25 and that negotiations had not resumed. She said regulators can, however, require carriers to maintain adequate networks and enforce statutory continuity-of-care protections.
Consumer protections and examples: Grant noted Maryland law currently provides 90 days of continuity-of-care protection for primary care and for complex conditions in some situations; she also reported that United re‑entered network with Capital Women's Care retroactive to Jan. 1 for that OBGYN provider. The administration plans regulatory updates to network adequacy standards and is proposing legislation to require earlier notice to consumers and the state when a large provider leaves a network, extend continuity-of-care protections (including behavioral health), and create a 90‑day special enrollment period for affected individual‑market enrollees.
Addressing market concerns: Grant said the MIA is monitoring whether carriers meet network adequacy rules and will use market-conduct investigations and carrier accountability reports to examine how insurers manage high-cost claimants. She also raised enforcement proposals aimed at curbing 'junk' or fraudulent plans, including penalties for third-party administrators when appropriate.
Provider claims of downcoding: Senators asked about reported increases in claim downcoding and inconsistent determinations. Grant said insurers are required to pay clean claims and the MIA is actively discussing whether the agency should issue clarifying guidance or bulletins to providers and payers; she indicated her team has been engaging providers directly about complaints.
Why it matters: Network disruptions can limit access to in‑network care and raise the risk of surprise bills or higher out-of-pocket costs. Grant argued that stronger notification rules and a short special enrollment window would reduce harm to consumers when large systems and insurers fall out of contract.
What’s next: Grant said the administration will advance departmental bills in committee next week and continue monitoring network adequacy and enforcement work. She also confirmed the MIA is staffing the state's adverse decisions commission and will share additional information as that group's work proceeds.
Quote: "We can make sure that our carriers have adequate networks, to serve their members," Grant said, summarizing the agency’s role.
The committee followed with questions about whether the United disputes signal a broader trend and pressed the MIA on issuing clarifying guidance for providers; Grant urged follow-up and said the agency would consider issuing bulletins or additional clarifications.
"As a regulatory agency, we can't force parties to contract," Grant said, recounting that the United–Johns Hopkins contract ended Aug. 25 and that negotiations had not resumed. She said regulators can, however, require carriers to maintain adequate networks and enforce statutory continuity-of-care protections.
Consumer protections and examples: Grant noted Maryland law currently provides 90 days of continuity-of-care protection for primary care and for complex conditions in some situations; she also reported that United re‑entered network with Capital Women's Care retroactive to Jan. 1 for that OBGYN provider. The administration plans regulatory updates to network adequacy standards and is proposing legislation to require earlier notice to consumers and the state when a large provider leaves a network, extend continuity-of-care protections (including behavioral health), and create a 90‑day special enrollment period for affected individual‑market enrollees.
Addressing market concerns: Grant said the MIA is monitoring whether carriers meet network adequacy rules and will use market-conduct investigations and carrier accountability reports to examine how insurers manage high-cost claimants. She also raised enforcement proposals aimed at curbing 'junk' or fraudulent plans, including penalties for third-party administrators when appropriate.
Provider claims of downcoding: Senators asked about reported increases in claim downcoding and inconsistent determinations. Grant said insurers are required to pay clean claims and the MIA is actively discussing whether the agency should issue clarifying guidance or bulletins to providers and payers; she indicated her team has been engaging providers directly about complaints.
Why it matters: Network disruptions can limit access to in‑network care and raise the risk of surprise bills or higher out-of-pocket costs. Grant argued that stronger notification rules and a short special enrollment window would reduce harm to consumers when large systems and insurers fall out of contract.
What’s next: Grant said the administration will advance departmental bills in committee next week and continue monitoring network adequacy and enforcement work. She also confirmed the MIA is staffing the state's adverse decisions commission and will share additional information as that group's work proceeds.
Quote: "We can make sure that our carriers have adequate networks, to serve their members," Grant said, summarizing the agency’s role.
The committee followed with questions about whether the United disputes signal a broader trend and pressed the MIA on issuing clarifying guidance for providers; Grant urged follow-up and said the agency would consider issuing bulletins or additional clarifications.
Don't Miss a Word: See the Full Meeting!
Go beyond summaries. Unlock every video, transcript, and key insight with a Founder Membership.
✓
Get instant access to full meeting videos
✓
Search and clip any phrase from complete transcripts
✓
Receive AI-powered summaries & custom alerts
✓
Enjoy lifetime, unrestricted access to government data
30-day money-back guarantee
